Discreet Shipping
From Venice Florida
Customer Support
support @ vagacare.com
Mon - Fri: 9:00 - 5:00
941-445-6005 | Online 24/7

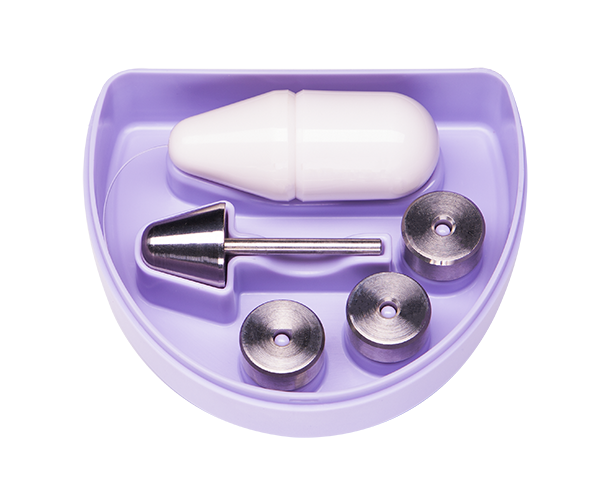
Vaginal weights are known also as kegel weights. They’re the most effective exercise system for strengthening weak pelvic muscles. Like bodybuilders, different weights target certain muscles. Designed to target pelvic floor muscles with gravity resistance. Require no electrical instrumentation or batteries. Above all, kegel weights can be used while walking, standing or laying. Additionally, their used throughout your day without interrupting your normal routine.
Our vaginal weights are:
In the first place, pelvic muscles are a group of ligaments in the pelvic floor. Otherwise, supporting the uterus and bladder. Secondly, these openings allow urine and bowel movements. Thirdly, attached to the tail bone. Most of all, without strong muscles situations can arise. This is where vaginal weights come in to play for strengthening. Using vaginal weights that strengthens pelvic floor muscles can have great benefits.
Weak muscles can result in:
Reference Links
There is a solution, it’s called Vagacare® vaginal weights. As a result, vaginal weights coupled with daily kegel exercises can improve weak muscles. Equally important, diet and exercise are both aspects of the recovery process. Eating healthier foods with fiber will also help to prevent constipation and improve straining. By the way, this system locates the correct muscle for you based on it’s design. It lays right were it’s needed, so no more guessing.
Don’t be a victim of weak vaginal muscles any longer. Take control, and enjoy the simple, normal freedoms of everyday life. Do you suffer from vaginal weakness? Buy our vaginal weights today, and start the recovery process. There’s no time like the present to make a life-changing decision. So then, the road to recovery starts now. But, if you don’t feel your muscles are weak, use the system anyway to make sure as you age they stay strong.
Vaginal weights can be used just about by every woman. All muscles in the body require a certain amount of work and exercise to maintain strength. Subsequently, through aging and neglect their overall use and function begin to decline. Furthermore, as we age, it is inevitable our muscles begin to breakdown and lose their elasticity.
Particularly, one group goes relatively unnoticed. Wherefore, its function is of great importance. The pubococcygeus (PF), or commonly referred as the pelvic floor, are a significant part of women’s anatomy and physiology. Many women are clueless when it comes to what their purpose is and how to strengthen them.
Understanding how kegel exercises improves elasticity and strength is the first step on the journey for self-improvement. Many preconceptions prevent women from utilizing specific devices for exercising. In the first place, those notions are things of the past. Women are taking back control and learning how easy it is to kegel exercise with kegel weights.
The purpose of the pubococcygeus muscle is to support the bodies core. This includes our digestive organs, uterus and aids in bladder and bowel functions. PM (pelvic muscle) is a neglected muscle, frequently going without exercise.
Our pelvic floor absorbs all the weight of our body and most woman do nothing about strengthening. Women don’t realize how weak they can become without proper exercise. Have you ever had to close your legs tight when you sneezed? Have difficulty achieving orgasm? Feel like your falling out down there? You are not alone! These are all signs that you are experiencing weak muscles. Most important, using kegel weights is the perfect way to achieve support.
Prolonged inactivity is one reason for loss of vaginal tone. The subject is often taboo and embarrassing to discuss. Don’t let that stop you! What we feel as age-appropriate behavior has a comical way to not apply to us as we approach our aging process.
Kegel exercising weights are ladies’ best friends, regardless of age, should be used. Younger aged women, can make sure they prevent muscles from declining. Most of all, older women will prolong the strength of theirs.
VagaCare® products are extremely effective in exercising the correct vaginal area. Easy to use and can be done while performing ordinary tasks around the house
Vaginal weights not only work out the PC muscles, they work out your whole core! The exercises that strengthen the pelvis and also strengthen; abdominal and lower back. Above all, improves core strength in general. Women that exercise their PM are less likely to suffer from age related issues later in life. Now is the time to start a kegel exercise program that targets your vaginal core.
Our bodies change throughout our lives and can affect multiple parts of our sexual and physical health. First of all, you and your partner may suffer from limited mobility and/or joint issues. Another fact is that the PC muscle function will decline with age. All women are affected by this issue. Thus, occurring at some point in their life. The situation is even more severe if you don’t exercise them. As a result, that’s why the product developed at VagaCare® remains a vital tool to help condition and strengthen while kegel exercising!
By the way, we already know the importance of working out major muscle groups. Legs, arms, and abs are just to name a few major groups. In this case, the forgotten muscles are the ones that get the least amount of attention, the PM (pelvic muscles). As a rule, science shows that as women age, muscles weaken over time, so take control! That’s why using VagaCare® is the way to go!
Stronger muscles make all the difference in a woman’s life. Generally, using kegel weights to strengthen the muscles provides more motivation than without aids. Just like in any exercise program, there is always a different level to reach and a harder task to accomplish.
Besides, kegel weights ensure the muscles are strengthened progressively. Above all, it just takes a few weeks using VagaCare®, you can reap the benefits of stronger muscles. Kegel exercising will improve your confidence. Working through the different size weights, you’ll feel self-assured in your increasing strength.
Exercising your PC with kegel weights makes a considerable difference in a woman’s general satisfaction and self-esteem. Your sex life should improve with a strengthened vaginal core. If you were having to cross your legs when sneezing, coughing, laughing or exercising, that will be a muscle weakness of the past. Like any other exercise program, your commitment will pay off with results.
Thereby, studies show that Kegel exercises steadily reinforce your vaginal core. VagaCare® is the best exerciser on the market. Championed by Medgo®’s 100% money back guarantee, now is the time to invest in kegel exercise weights. So then, all you must do is to start slow, follow our guidelines. Enjoy exercising with confidence.
From Venice Florida
support @ vagacare.com
941-445-6005 | Online 24/7
* 100% Discreet Shipping
* Secure Shopping
* Trusted for 12 Years
* No Catalogs Mailed to Your Home
* Real People That Care About You
Call: 941.445.6005
© COPYRIGHT 2006-2018 VagaCare® an Affiliate of Medgo® LLC. ALL RIGHTS RESERVED.
Our Healthy products are not intended to diagnose, cure or prevent any disease.